Table of Contents
- 1 Ayahuasca and Depression: Benefits, Dangers, and What the Science Really Says
- 1.1 What Ayahuasca Is, Briefly
- 1.2 Ayahuasca and Depression: What the Clinical Evidence Shows
- 1.3 How Ayahuasca Affects the Depressed Brain
- 1.4 The Real Dangers, Not the Footnoted Ones
- 1.5 Post-Ayahuasca Depression: The Dark Night Few People Warn You About
- 1.6 Ayahuasca Compared: Psilocybin, Ketamine, SSRIs
- 1.7 The Legal Reality
- 1.8 How To Decide Safely
- 1.9 Frequently Asked Questions
- 1.10 Conclusion
- 1.11 References
Ayahuasca and Depression: Benefits, Dangers, and What the Science Really Says
| Question | Short answer |
|---|---|
| Does the science support it? | Two RCTs in treatment-resistant depression; a meta-analysis of 126 studies ranks ayahuasca second only to psilocybin among major psychedelics (Yao et al., 2024) |
| How fast does it work? | Antidepressant effects measurable within hours to days of a single supervised dose (Palhano-Fontes et al., 2019) |
| Safe with antidepressants? | No. SSRIs, SNRIs, MAOIs, lithium, tramadol, and several others require a supervised washout to avoid serotonin syndrome (Callaway & Grob, 1998) |
| Hard contraindications? | Bipolar disorder, primary psychotic disorders, severe cardiovascular disease, current pregnancy, active eating disorders |
| Legal in the US? | DMT is Schedule I federally; religious exemption for specific churches; state-level decriminalization in Colorado (Gonzales v. UDV, 2006) |
Depression that has not responded to two or more antidepressant trials is a different problem than depression that lifts on the first SSRI a clinician prescribes. The evidence below speaks mostly to that first group, the patients for whom standard care has not worked. Read it as a map of what is known and what is not, drawn from the strongest sources available rather than from retreat marketing.
What Ayahuasca Is, Briefly
The pharmacology is older than any of the modern claims about it.
Ayahuasca is a brew made from two Amazonian plants. The vine Banisteriopsis caapi carries a class of alkaloids called β-carbolines (harmine, harmaline, tetrahydroharmine) that inhibit the enzyme monoamine oxidase A. The leaf Psychotria viridis, or in the Colombian Putumayo Diplopterys cabrerana, carries N,N-dimethyltryptamine, or DMT.
DMT is broken down too quickly in the gut to be active when swallowed alone. The β-carbolines block that breakdown. Together the two plants make oral DMT possible (Egger et al., 2024). This combination is why ayahuasca works in the body when chewed leaves of either plant alone do nothing. It is also why the safety profile is harder than psilocybin’s. The MAOI half of the brew interacts with foods and medications. We come back to that in section four.
For a fuller account of the brew’s botany, lineage, and ceremonial context, see our overview of ayahuasca.
Ayahuasca and Depression: What the Clinical Evidence Shows
Most of the strongest evidence sits in two trials and one meta-analysis.
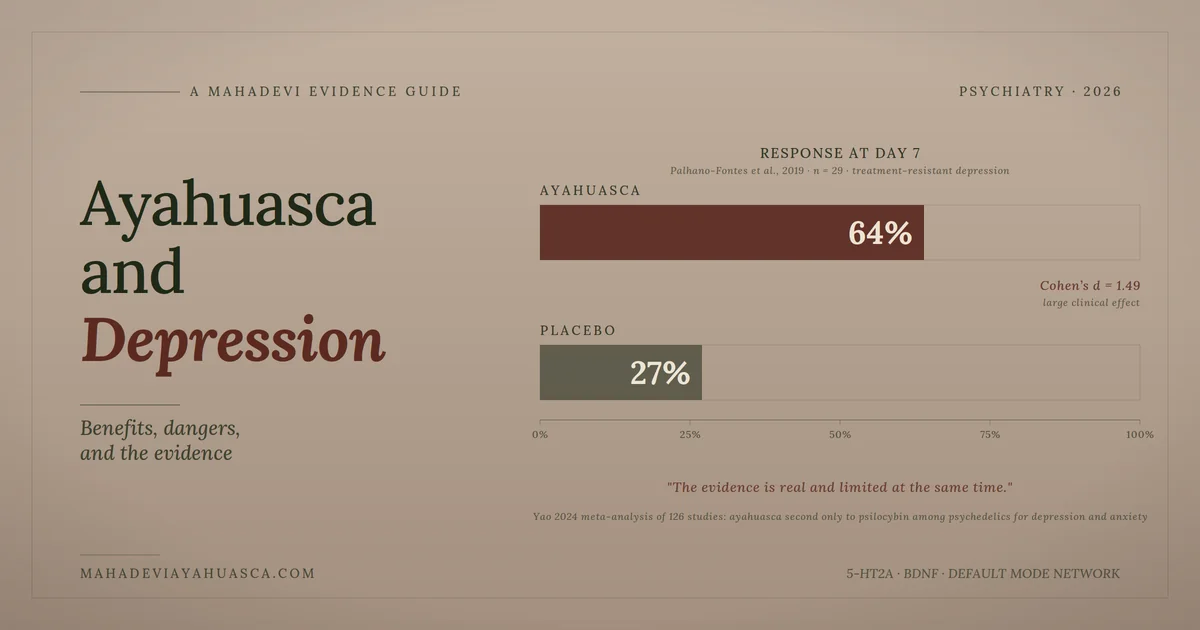
The cleanest piece of evidence is a 2019 randomized, placebo-controlled trial conducted at the Brain Institute in Natal, Brazil. Twenty-nine patients with treatment-resistant depression received either a single dose of ayahuasca or a sensory-matched placebo. Response rates at day seven were 64 percent in the ayahuasca arm against 27 percent for placebo, with a between-group effect size of Cohen’s d = 1.49 on the MADRS depression scale (Palhano-Fontes et al., 2019). The same dataset was reanalyzed for suicidal ideation. Within-group reductions were large in the ayahuasca arm at every time point through day seven (Zeifman et al., 2019).
Earlier open-label work pointed in the same direction. A 2015 trial in patients with recurrent depressive disorder showed fast antidepressant and anxiolytic effects within hours of a single dose (Osório et al., 2015). A 2016 SPECT-imaging study in the same population confirmed the clinical effect and tied it to changes in brain perfusion (Sanches et al., 2016).
The largest synthesis to date is a 2024 systematic review and meta-analysis of 126 articles. It placed ayahuasca second only to psilocybin among major psychedelics for depression and anxiety, with a Hedges’ g of -1.34 (Yao et al., 2024). That is a large effect by any clinical standard. The most common side effect across studies was headache.
Observational data is less rigorous but much larger. The Global Ayahuasca Project, an international cross-sectional survey of 11,912 ayahuasca users, found that 78 percent of respondents with prior depression diagnoses described their symptoms as very much improved or completely resolved after ayahuasca consumption (Sarris et al., 2021). Self-report has limits. People who feel better answer surveys. People who do not feel better, or who got worse, drop off. Read the number with that in mind.
Two RCTs, several open-label trials, one large meta-analysis, and a self-selected survey of nearly 12,000 people. That is the evidence base for ayahuasca and depression as it stands. It is the strongest case for any psychedelic short of psilocybin. It is also smaller than the evidence base for SSRIs by orders of magnitude. Both are true.
How Ayahuasca Affects the Depressed Brain
Three mechanisms keep showing up across the imaging and biomarker work.
The first is the serotonin system. DMT is a partial agonist at the 5-HT2A receptor, the same receptor that psilocybin and LSD bind. Activation here is the entry point for the acute psychedelic state and, on most current models, for the antidepressant signal as well (Egger et al., 2024).
The second is neuroplasticity. A 2019 placebo-controlled trial measured serum brain-derived neurotrophic factor (BDNF) before and after a single dose. BDNF rose significantly in both depressed patients and healthy controls compared to placebo, and BDNF levels in the depressed arm correlated inversely with depression scores (de Almeida et al., 2019). A 2021 systematic review found the same neuroplastic signal across psychedelics generally (de Vos et al., 2021). Whatever the brew is doing at the cellular level, it moves things that matter for how brains change.
The third is the default mode network, the brain’s resting self-referential system. Ayahuasca decreases activity and connectivity within this network during the acute experience and changes its connectivity to the salience network for at least 24 hours afterward (Palhano-Fontes et al., 2015; Pasquini et al., 2020). Hyperactive default mode network activity is one of the more replicated findings in depression research. Quieting it, even temporarily, may be part of why patients describe the experience as stepping outside their depression rather than simply pushing through it.
There is also a peripheral piece. A 2020 RCT showed C-reactive protein, a marker of systemic inflammation, dropping significantly within 48 hours of a single dose. The drop was larger in patients who had larger reductions in depressive symptoms (Galvão-Coelho et al., 2020). Inflammation and depression are linked in ways the field is still working out. Ayahuasca seems to act on both ends of that link at once.
None of these mechanisms is settled. They overlap. They are best read as pieces of a larger picture rather than as a single explanation (Rossi et al., 2022).
The Real Dangers, Not the Footnoted Ones
The most serious risk in this entire conversation is a drug interaction most retreats fail to screen for properly.
The MAOI in ayahuasca is the safety problem. It is a reversible MAO-A inhibitor, which is why the effect window is hours rather than weeks, but during those hours the body cannot metabolize serotonin the way it normally does. Add a serotonin reuptake inhibitor, which covers most SSRIs and SNRIs in current use, and you risk serotonin syndrome. The clinical syndrome runs from agitation, fever, and tremor to seizures and death (Callaway & Grob, 1998; Ruffell et al., 2020).
This is not a hypothetical. The pharmacology is well documented. The standard recommendation, repeated across harm-reduction literature, is a washout window before any ayahuasca exposure: roughly two weeks for most SSRIs, six weeks for fluoxetine because of its long half-life, and longer for MAOIs themselves. Any washout has to be supervised by the prescribing clinician. Coming off antidepressants on your own to attend a retreat is a separate category of bad idea. For the full breakdown of agents, half-lives, and what supervised tapers look like, see our dedicated SSRI and MAOI interaction guide.
Other contraindications are firmer than retreat brochures usually admit:
- Bipolar disorder. Ayahuasca’s antidepressant action can precipitate mania in predisposed individuals. A documented case report describes a patient with undiagnosed bipolar disorder developing a full manic episode with psychotic features within two days of completing a four-day ayahuasca ritual (Szmulewicz et al., 2015). See ayahuasca and bipolar disorder for the deeper guide.
- Personal or family history of primary psychotic disorders. A systematic review of post-ayahuasca psychotic episodes found that almost every documented case involved someone with a personal or family history of a psychotic or manic disorder. Pre-screening reduces this risk substantially (dos Santos et al., 2017). For deeper coverage, see ayahuasca and psychosis risk.
- Serious cardiovascular disease. Ayahuasca acutely raises blood pressure; in controlled study, the diastolic rise of about 9 mmHg at 75 minutes reached statistical significance, while systolic and heart-rate rises were moderate but non-significant (Riba et al., 2003). See also our deeper guides on ayahuasca and blood pressure and ayahuasca and the heart.
- Pregnancy. Animal studies show developmental toxicity at doses above the human ceremonial range, with maternal mortality and fetal anomalies in pregnant rats (Motta et al., 2018).
The Global Ayahuasca Survey, the largest safety dataset to date with 10,836 participants from over 50 countries, found acute physical adverse effects in 69.9 percent of users, mostly vomiting, which is part of the experience. Only 2.3 percent required medical attention. Adverse mental health effects in the weeks or months following use were reported by 55.9 percent, though about 88 percent of those who experienced them described them as part of a positive growth process (Bouso et al., 2022).
The honest reading: serious medical events are rare in screened, supervised settings. The risk profile changes when the screening is sloppy or the setting is unregulated. The U.S. Embassy in Lima updated its advisory after multiple American deaths at unregulated Peruvian retreats (U.S. Embassy Lima, 2025). The medicine is not the only variable. The infrastructure around it is.
Post-Ayahuasca Depression: The Dark Night Few People Warn You About
Some of the most difficult mental health effects show up after the ceremony, not during it.
The same Global Ayahuasca Survey that documented the physical safety profile also tracked what happened in the weeks and months after. Just over half of participants reported some kind of difficult mental health effect post-ceremony. Most framed these effects as part of growth. A meaningful minority did not (Bouso et al., 2022).
The difficult effects can take several shapes. A re-emergence of depression that had lifted in the days after the ceremony. A wave of grief or anger as buried material surfaces. Anxiety that persists for weeks. A flatness that sits in the place where the afterglow used to be. Some people describe what the contemplative literature has long called a dark night: a period of disorientation that follows opening rather than fixing.
Two pieces of evidence matter here. The first is qualitative. A large analysis of integration experiences specifically among ayahuasca drinkers, drawing on 1,630 respondents from a global survey, found that integration was experienced as challenging, long-term, and communal rather than primarily individual (Cowley-Court et al., 2023). The clinical model of one-on-one psychotherapy after a ceremony is not what most ayahuasca drinkers actually rely on for integration. They rely on community, on time, and on repeated practice.
The second is timing. Acute antidepressant effects in the controlled trials are real at one week. Less is known about how long they hold for any individual patient. Risk factors for poorer post-ceremony outcomes include unsupervised settings, prior psychiatric diagnoses, lower-quality preparation, and weak integration support (Perkins et al., 2021).
The piece of advice that most ayahuasca-experienced clinicians repeat: budget more time for after than for before. The week of preparation is shorter than the months of integration. If you cannot give the integration period the weight it needs, postpone the ceremony.
Ayahuasca Compared: Psilocybin, Ketamine, SSRIs
Different mechanisms, different risk profiles, different roles.
A 2024 Bayesian network meta-analysis published in The BMJ compared psilocybin, LSD, MDMA, ayahuasca, and escitalopram across 19 RCTs for depression. Among the psychedelics studied, only high-dose psilocybin showed superiority over a well-blinded antidepressant placebo. Ayahuasca showed benefits within psychedelic trial conditions, and all agents were generally well tolerated (Hsu et al., 2024). An earlier systematic review reached a similar conclusion: ayahuasca, psilocybin, and LSD all show antidepressant, anxiolytic, and anti-addictive signals across small clinical trials (dos Santos et al., 2016).
| Treatment | Mechanism | Onset | Acute duration | Evidence base | Key risk |
|---|---|---|---|---|---|
| Ayahuasca | DMT plus reversible MAO-A inhibition; 5-HT2A; BDNF; default mode network modulation | 30 to 60 min | 4 to 6 hours | Two RCTs in TRD; meta-analysis Hedges’ g = -1.34; large observational data | Serotonin syndrome with SSRIs, SNRIs, MAOIs; psychiatric contraindications |
| Psilocybin | 5-HT2A agonist; default mode network modulation | 20 to 40 min | 4 to 6 hours | Multiple RCTs; FDA Breakthrough Therapy designation | Bad trip; rare HPPD; same psychiatric contraindications as ayahuasca |
| Ketamine / esketamine | NMDA receptor antagonism | Minutes (IV); ~40 min (intranasal) | 40 to 60 min | Largest psychedelic-adjacent evidence; FDA-approved (Spravato) | Dissociation; bladder toxicity with frequent use; addiction potential |
| SSRIs | Serotonin reuptake inhibition | 4 to 6 weeks for full effect | Continuous daily dosing | The largest evidence base of any depression treatment | Sexual side effects; suicidality risk in young patients; discontinuation syndrome |
A few practical notes on the table. Esketamine has FDA approval as a nasal spray (Spravato) for treatment-resistant depression in supervised clinical settings. SSRIs remain first-line for most depression presentations and have, by orders of magnitude, the largest evidence base. Psilocybin has the strongest psychedelic evidence to date and the cleanest pharmacological profile, with no MAOI-class drug interactions. Ayahuasca’s evidence is real and smaller. Its drug interaction profile is the hardest of the four.
None of this is a recommendation to choose one over another. Treatment selection is a clinical conversation, not a search-result decision. The point of the comparison is to show that ayahuasca sits inside a landscape, not outside it.
The Legal Reality
DMT is Schedule I. Almost all of the legal nuance flows from there.
DMT is a Schedule I controlled substance in the United States under the Controlled Substances Act, classified alongside heroin and LSD as having no accepted medical use and high abuse potential (DEA Diversion Control Division, 2024). Ayahuasca, which contains DMT, falls under the same federal prohibition unless a specific exemption applies.
The two main federal exemptions both come from religious-freedom litigation. The 2006 unanimous Supreme Court ruling in Gonzales v. O Centro Espírita Beneficente União do Vegetal held that the Religious Freedom Restoration Act protects the União do Vegetal church’s sacramental use of ayahuasca (Gonzales v. UDV, 546 U.S. 418, 2006). A subsequent court settlement extended similar protection to specific Santo Daime congregations. These are the only standing federal religious exemptions for ayahuasca in the U.S.
State law has begun to move. Colorado’s Proposition 122, the Natural Medicine Health Act passed in 2022, decriminalized personal use of five natural psychedelics for adults 21 and older, including DMT. Colorado licensed healing centers may offer supervised DMT sessions in phased rollout, subject to state Natural Medicine Advisory Board approval (Colorado Natural Medicine Health Act, 2022). Federal law does not change because of this. Schedule I is Schedule I.
Outside the U.S. the picture is patchwork. Brazil legally recognizes religious ayahuasca use through CONAD Resolution 1/2010. Peru has declared traditional ayahuasca use part of its national cultural patrimony (INC Peru, 2008). The Netherlands ended its long-standing Santo Daime exemption with a 2019 Supreme Court ruling that the Opium Act takes precedence over religious freedom (ICEERS, 2023). Colombia has no specific legislation either way and recognizes yagé under broad cultural protections (Suárez, ICEERS, 2023).
For most readers, the practical question is travel. Foreign retreats operate inside a legal framework different from the one the traveler returns to. Whether any of this is legal where you live is a separate question from the one most people ask first.
How To Decide Safely
If a retreat will not screen you, it will not catch you.
The single largest predictor of a serious adverse event is participation in an unsupervised setting with inadequate screening (Bouso et al., 2022). Most of the safety conversation comes down to whether the screening is real or for show.
A real screening process asks for your full medication list, your psychiatric history, your family psychiatric history, your cardiovascular history, and a recent physical. It declines participants with bipolar disorder, schizophrenia or schizoaffective disorder, current psychosis, severe cardiovascular disease, current pregnancy, or active eating disorders. It requires a documented washout from any contraindicated medication, supervised by the prescribing clinician. It does not allow last-minute additions. It does not let a participant talk their way past a contraindication.
Red flags to watch for in any retreat or church:
- No medical screening, or screening done only after payment
- Pressure to come off medications without specifying who supervises the washout
- Vague or absent integration support after the ceremony
- Facilitator credentials that cannot be verified
- Group sizes large enough that one-on-one attention during the ceremony is impossible
- Reassurance that “the medicine will sort it out” in response to specific medical questions
The ICEERS Better Practices guide, commissioned by the Catalan Department of Health, sets out a workable baseline screening framework that any responsible retreat or church can match or exceed (ICEERS, 2019). Survey work on ceremonial context found that setting quality, especially leadership and social dimensions, predicted both better mystical experience scores and lower scores on challenging-experience measures (Perkins et al., 2021). The container does work the medicine cannot do on its own.
Integration matters as much as preparation. Plan for at least a few weeks of reduced commitments after the ceremony. Find a therapist, a community, or an integration practitioner before you go, not after. The peer-reviewed literature now treats integration as a standalone clinical practice with its own protocols (Gorman et al., 2021; Greń et al., 2023).
If you are reading this as a person with depression, the question to ask yourself is not whether ayahuasca might help. It probably could. The question is whether your specific situation has the medical clearance, the setting, and the post-ceremony support to give the medicine a fair chance to do its work without making things worse.

Feel deeply.
Show up fully.

About the Author
Yasha Shah is the founder of MahaDevi Ayahuasca, a retreat center in Colombia. He has been working with ayahuasca since 2017, with experience across hundreds of ceremonies as both a participant and retreat organizer. Trained within the Shipibo and Camsá traditions, his work bridges indigenous wisdom, harm-reduction principles, and practical integration for modern seekers. Yasha writes about ayahuasca, plant medicine, and psychedelics, covering integration, preparation, and harm reduction to help readers make informed and responsible decisions.
Frequently Asked Questions
Can ayahuasca cause depression?
Some people experience a flat or low period in the days or weeks after a ceremony. This is more often described as part of integration than as a relapse, but the difference matters when it lasts. Risk factors for a difficult post-ceremony period include unsupervised settings, prior psychiatric diagnoses, weak preparation, and limited integration support (Bouso et al., 2022). If a low period is not lifting after a few weeks, that is a clinical situation, not a spiritual one.
Can ayahuasca cure depression?
No psychedelic has been shown to cure depression. The strongest evidence to date shows rapid, large reductions in depression scores after a single supervised dose, with effects measurable at one week and partial maintenance over months in some patients (Palhano-Fontes et al., 2019). A meta-analysis of 126 studies found a large overall effect size for ayahuasca on depression and anxiety (Yao et al., 2024). This is meaningful clinical signal, not a cure.
Is ayahuasca safe for people on antidepressants?
No. The MAOI in the brew interacts with serotonergic medications including SSRIs, SNRIs, MAOIs, tramadol, lithium, and several others, with serotonin syndrome a real and documented risk (Callaway & Grob, 1998). Any medication change before a ceremony has to be planned with the prescribing clinician and properly timed. A two-week washout is typical for most SSRIs; fluoxetine requires longer because of its long half-life. See our SSRI and MAOI interaction guide for the full breakdown.
How long can post-ayahuasca depression last?
It varies. Most difficult mental health effects in the weeks after a ceremony resolve with time, integration support, and community. A minority of users describe symptoms that persist for months (Bouso et al., 2022). If post-ceremony symptoms are interfering with daily function past a few weeks, work with a mental health professional rather than waiting for them to lift on their own.
Can ayahuasca cause psychosis or a bad trip you do not recover from?
Documented psychotic episodes after ayahuasca are rare in screened populations, with estimates ranging from 0.0032 to 0.096 percent in long-running ayahuasca church samples. Almost every documented case involved a personal or family history of psychotic or manic disorder (dos Santos et al., 2017). Adequate pre-screening removes most of this risk. Skipping pre-screening does not.
How does ayahuasca compare to ketamine or psilocybin for depression?
Different mechanisms, different evidence bases, different risk profiles. Ketamine works on the NMDA receptor and is the only one of the three with FDA approval (esketamine, as Spravato). Psilocybin has the strongest psychedelic evidence base and a cleaner pharmacological profile (Hsu et al., 2024). Ayahuasca has real but smaller evidence and the hardest drug-interaction profile of the three.
Is ayahuasca legal in the United States?
DMT is Schedule I federally (DEA, 2024). The only standing federal exemptions are religious, granted to specific churches following Gonzales v. UDV (2006). Colorado’s Natural Medicine Health Act decriminalized personal possession of DMT among other natural psychedelics, with licensed healing centers in phased rollout (Colorado Prop 122, 2022). State law does not change federal law.
Does ayahuasca show up on a drug test?
Standard workplace drug panels (5-panel, 10-panel) do not include DMT or its metabolites. Specialized GC/MS or LC/MS panels can detect DMT in blood or urine for a short window, typically less than 24 hours, but these are rarely ordered outside of forensic or research contexts.
What should I look for in a safe ayahuasca retreat for depression?
Real medical screening before payment, refusal to accept participants with hard contraindications, supervised washout requirements for any psychiatric medications, integration support included rather than upsold, facilitator credentials that can be verified, and group sizes small enough that one-on-one attention is realistic (ICEERS, 2019). A retreat that will not screen you will not catch you if something goes wrong.
How many ceremonies does it take to see results in depression?
The clinical trials measured effects after a single supervised dose (Palhano-Fontes et al., 2019). Most ceremonial settings include three to seven ceremonies over a week. There is no published evidence that more is better for depression specifically, and there is good reason to believe that what happens between ceremonies (rest, integration, time) carries much of the therapeutic weight.
Conclusion
The clinical evidence is real. The risks are real. The cultural and ceremonial container around the medicine is older and more sophisticated than most Western readers know, and it does work the chemistry cannot do alone.
What ayahuasca is not: a faster antidepressant, a vacation cure, a substitute for the slow work of getting better.
What it is, when the screening is real and the setting is right and the integration is taken seriously, is one of the most powerful tools available for moving treatment-resistant depression in a direction it has not moved in years.
Most of what determines the outcome happens before and after the ceremony, not during it.
The medicine is part of the answer. It is not the answer.
References
Gonzales v. O Centro Espírita Beneficente União do Vegetal, 546 U.S. 418 (2006).
Domsac I, Russo S, Sánchez Avilés C / ICEERS. (2023). Legal Status of Ayahuasca in the Netherlands.
U.S. Embassy Lima, Peru. (2025). Health Alert: Do Not Use Ayahuasca/Kambo. U.S. Department of State.


