Table of Contents
- 1 Ayahuasca and Schizophrenia: What the Evidence Says About Risk, Safety, and Screening
- 1.1 What Ayahuasca Is, and What It Does in the Brain
- 1.2 Why Ayahuasca and Schizophrenia Get Mentioned in the Same Sentence
- 1.3 Can Ayahuasca Cause or Trigger Schizophrenia?
- 1.4 Family History: The Risk Factor Most People Skip
- 1.5 Can Ayahuasca Treat or Cure Schizophrenia?
- 1.6 Contraindications, Drug Interactions, and Who Should Not Drink
- 1.7 Spiritual Emergency vs Psychotic Break: How to Tell the Difference
- 1.8 How Ethical Retreats Screen, and What to Look For
- 1.9 Frequently Asked Questions
- 1.10 Conclusion
- 1.11 References
Ayahuasca and Schizophrenia: What the Evidence Says About Risk, Safety, and Screening
| Question | Answer | What the evidence says |
|---|---|---|
| Can ayahuasca trigger psychosis in vulnerable people? | Yes | Documented in a systematic review of human studies; most cases involved personal or family history of psychotic or manic disorders (dos Santos et al., 2017). |
| Can ayahuasca cure or treat schizophrenia? | No | No registered clinical trials in schizophrenia. Not a recognized treatment indication. |
| Is a family history of psychosis a contraindication? | Yes | First-degree relative with a psychotic disorder is a standard exclusion criterion in clinical and harm-reduction guidelines (Rossi et al., 2023; ICEERS, 2019). |
| Are unsupervised settings riskier? | Yes | Non-supervised context and pre-existing psychiatric diagnosis were the strongest predictors of adverse mental health effects in the largest survey to date (Bouso et al., 2022). |
The honest version of this conversation has three parts. First, what ayahuasca actually does in the brain, and why that overlaps with the symptom geography of psychosis. Second, what the case reports and the systematic reviews tell us about who has been hurt. Third, what a careful prospective participant, or a family member trying to stop one, can do with that information. The piece below covers each in turn, with citations to the studies that the screening protocols of reputable retreats already rely on.
What Ayahuasca Is, and What It Does in the Brain
A brew, a vine, a leaf, and a piece of pharmacology that should not work but does.
Ayahuasca is a decoction. Two plants, simmered together for hours: the woody vine Banisteriopsis caapi, and the leaf of either Psychotria viridis in Peruvian and Brazilian traditions or Diplopterys cabrerana in much of Colombia and Ecuador (Brito-da-Costa et al., 2020). The leaf supplies N,N-dimethyltryptamine, or DMT. The vine supplies the β-carboline alkaloids harmine, harmaline, and tetrahydroharmine (Callaway, Brito, & Neves, 2005).
Without the vine, the leaf is inert orally. DMT is a powerful 5-HT2A receptor agonist, but the gut and liver destroy it on first pass through the enzyme monoamine oxidase A. The β-carbolines in the vine inhibit that enzyme just long enough to let the DMT cross into circulation, reach the brain, and bind (Egger et al., 2024; Ruffell et al., 2020). That is the entire trick. A leaf that does nothing on its own, paired with a vine that lets it do everything.
What the reader needs to understand for the rest of this piece is that ayahuasca is, in pharmacological terms, two drugs at once. A serotonergic psychedelic and a reversible MAO inhibitor. The dual mechanism is what makes ayahuasca distinct among psychedelics, and it is also what makes the safety conversation different from the one you would have about psilocybin or LSD. For a fuller treatment of the brew itself, the lineages, the brewing, and the ceremony, see our overview of ayahuasca as a plant medicine.
Why Ayahuasca and Schizophrenia Get Mentioned in the Same Sentence
Some of what ayahuasca does looks like what schizophrenia does. The overlap is not metaphor. It is receptor-level.
The classic psychedelics produce a state that researchers since the 1950s have called “model psychosis.” Visual perception breaks open. The boundary between self and not-self softens or vanishes. Thought becomes associative in ways that, on a clinician’s checklist, look like loose associations or formal thought disorder. The mechanism shares ground with what is happening in an active psychotic episode, particularly through 5-HT2A receptor agonism and downstream glutamate activity (Frecska, Bokor, & Winkelman, 2016).
For most people in good psychiatric standing, the state is bounded. It begins, peaks, and ends. The brain returns to baseline within four to six hours. The β-carbolines have already been metabolized. By the next morning the person is sore, tired, often grateful, often quiet, but back.
For some people the state does not end on schedule. The visions persist. The associative thinking continues. What was supposed to be a single ceremony becomes a psychotic episode requiring hospitalization. The systematic review of every published human case of ayahuasca-associated psychosis found that in nearly every documented case, the person had a personal or family history of psychotic or manic illness (dos Santos et al., 2017). The medicine did not invent the vulnerability. It surfaced it.
Can Ayahuasca Cause or Trigger Schizophrenia?
The honest words here are not “cause” or “cure.” They are “trigger” and “unmask.”
Schizophrenia is a complex disorder with substantial heritability and a developmental arc that begins long before symptoms become visible. The diathesis-stress model, which most clinical psychiatry runs on, holds that the disorder emerges when an underlying vulnerability meets a sufficient environmental stressor. Vulnerability is largely set. Timing belongs to the stressor.
Ayahuasca is, for a vulnerable brain, a profound stressor. A 6-hour direct activation of the same receptor systems that misfire in psychosis. In someone whose first-episode psychosis was going to arrive at age 24, ayahuasca at 23 may be the trigger that pulls it forward. The medicine does not write the script. It pushes a play button that was already loaded.
This is what the published case reports describe. A young man with no prior psychiatric diagnosis, but with a family history of bipolar illness, attends a 4-day ayahuasca ritual in Brazil and develops a full manic episode with psychotic features that persists well past the half-life of the β-carbolines, meeting DSM criteria for bipolar I (Szmulewicz et al., 2015). The systematic review identifies similar patterns across the broader literature: rare in absolute terms, with estimates of 0.0032 to 0.096% of União do Vegetal servings producing a psychotic episode, but concentrated almost entirely in people with personal or family histories of psychotic or manic disorders (dos Santos et al., 2017). For deeper coverage, see our companion guides on ayahuasca and psychosis risk and ayahuasca and bipolar disorder.
The numbers are small. What happens to the people inside them is not. A first psychotic episode reorganizes a life, and the ones triggered by psychedelic exposure can be slower to resolve and harder to treat than ones that emerge endogenously. The math of the research community has been clear for decades: screen out the vulnerable, and the medicine becomes meaningfully safer for everyone else.
Family History: The Risk Factor Most People Skip
A first-degree relative with a psychotic disorder is the single most useful piece of information you can give a screener. Most prospective participants have never been asked.
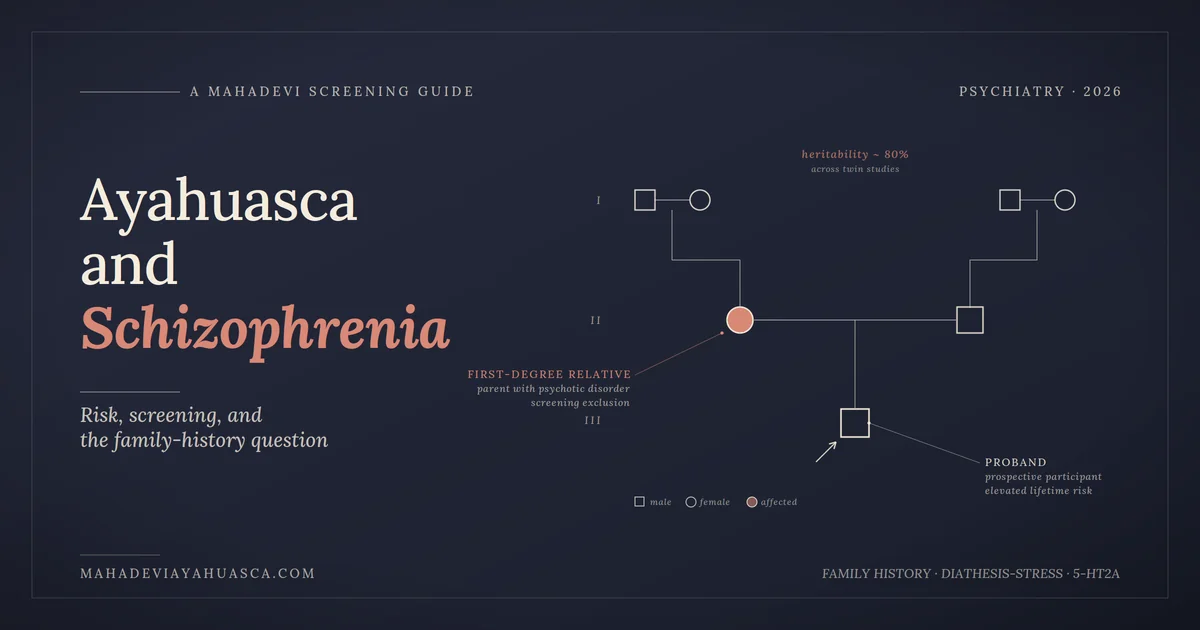
The screening protocols used in clinical ayahuasca research and recommended by harm-reduction organizations all converge on the same exclusion: a first-degree relative (parent, sibling, or child) with a diagnosis of schizophrenia, schizoaffective disorder, bipolar I with psychotic features, or other primary psychotic illness (Rossi et al., 2023; ICEERS, 2019). The reasoning is the heritability data. Schizophrenia heritability sits at roughly 80% across twin studies, and first-degree relatives of an affected proband carry a meaningfully elevated lifetime risk compared with the general population.
The question that prospective participants tend to underestimate is whether to disclose. There is sometimes a worry, often unspoken, that a family history will simply disqualify them. It often will. That is the point. The retreats that take this seriously would rather lose a participant to a careful “no” than gain one to a preventable crisis.
If the family history is unclear, two questions are usually enough to surface it. First: Has anyone in your immediate family been hospitalized for mental illness, or treated long-term with antipsychotic medication? Second: Has anyone in your immediate family been told they had a “breakdown,” “nervous collapse,” or a period of believing things that turned out not to be real? The second question catches what the first one misses, because earlier generations rarely received formal diagnoses but often received the experience.
Can Ayahuasca Treat or Cure Schizophrenia?
No. The studies people sometimes cite are about other conditions entirely.
There are no registered clinical trials of ayahuasca as a treatment for schizophrenia. The mechanism that gives ayahuasca its therapeutic profile in other conditions, sustained 5-HT2A receptor activation with downstream effects on neuroplasticity and inflammation, is the same mechanism that makes it dangerous in schizophrenia. You cannot use the brew as antidote and accelerant at once.
What the research does support, in carefully selected populations that explicitly exclude psychotic illness, is therapeutic potential for treatment-resistant depression. A randomized placebo-controlled trial of a single dose of ayahuasca in 29 patients with treatment-resistant depression reported response rates of 64% versus 27% at one week, with a between-group effect size of d = 1.49 (Palhano-Fontes et al., 2019). Systematic reviews of clinical trials of ayahuasca, psilocybin, and LSD describe consistent antidepressant, anxiolytic, and anti-addictive signals across studies (dos Santos et al., 2016). Every one of those trials excluded participants with personal or family histories of psychotic illness as a baseline safety condition. For more on the depression evidence base specifically, see our guide on ayahuasca for depression.
This is the distinction the wellness internet collapses and the science does not. Ayahuasca is being studied for several psychiatric conditions. Schizophrenia is not on the list, and there is no credible scientific path on which it will become one in the foreseeable future. Anyone marketing ayahuasca as a treatment for schizophrenia is either uninformed or unscrupulous.
Contraindications, Drug Interactions, and Who Should Not Drink
The pharmacology that makes ayahuasca work also makes it dangerous around several common medication classes. The schizophrenia conversation lives inside this larger map.
Reversible MAO-A inhibition, the mechanism that lets oral DMT reach the brain, is also the mechanism that makes ayahuasca interact badly with serotonergic and certain sympathomimetic medications. The interaction with selective serotonin reuptake inhibitors, the most commonly prescribed class of antidepressants, is the most clinically important: combining the two creates a real risk of serotonin syndrome, a potentially life-threatening condition (Callaway & Grob, 1998; Ruffell et al., 2020). The risk is not theoretical. A serotonin syndrome case has been published involving fluoxetine and ayahuasca. For washout windows by drug class, see our SSRI and MAOI interaction guide.
The table below summarizes the major medication and condition contraindications drawn from clinical pharmacology reviews and harm-reduction guidelines. It is not exhaustive. It is the floor.
| Substance or condition | Risk | Severity tier |
|---|---|---|
| Schizophrenia or other primary psychotic disorder | Triggering or prolonging psychotic episode; symptom worsening | Avoid |
| First-degree relative with psychotic disorder | Diathesis-stress activation; first-episode psychosis risk | Avoid |
| Bipolar I or II with manic history | Switch into mania, including with psychotic features | Avoid |
| SSRIs (fluoxetine, sertraline, escitalopram, others) | Serotonin syndrome | Avoid; long washout required, supervised by prescriber |
| SNRIs, TCAs, MAOIs, lithium, trazodone | Serotonin syndrome, hypertensive crisis, mania | Avoid; washout and prescriber consultation |
| Tramadol, dextromethorphan, methadone, linezolid, triptans, St. John’s wort | Serotonin syndrome | Avoid (Malcolm & Lee, 2018) |
| Severe or uncontrolled hypertension; recent cardiac event | Acute blood pressure rise (roughly 10 to 35 mmHg systolic); cardiovascular strain | Avoid (Riba et al., 2003) |
| Pregnancy | Animal models show abortifacient and teratogenic effects at higher doses | Avoid (White et al., 2024) |
| Active suicidality without integrated psychiatric care | Acute crisis without containment; intensification of distress | High caution; do not attend without coordinated care |
| Tyramine-rich foods within 24 hours pre-ceremony | Hypertensive interaction via residual MAO inhibition | Discuss with retreat; follow dieta |
The cardiovascular numbers in the table are not theoretical either. A controlled pharmacology study in healthy volunteers found a statistically significant diastolic rise of about 9 mmHg at 75 minutes after the high dose; the parallel systolic and heart-rate rises were moderate and not statistically significant, and all values resolved within four hours (Riba et al., 2003). Other studies have reported larger transient rises in some participants. For a healthy 35-year-old, this is unremarkable. For someone with existing cardiovascular vulnerability, it is the reason that any retreat worth attending will check blood pressure history before pouring. See also our deeper guides on ayahuasca and blood pressure and ayahuasca and the heart.
Spiritual Emergency vs Psychotic Break: How to Tell the Difference
Both can be intense. Both can include unusual experiences. The clinical questions are about reality testing, response to support, and what happens when the medicine wears off.
Ayahuasca ceremonies routinely produce material that, on a flat clinical reading, looks similar to active psychotic content. Visions of beings. Reorganizations of personal history. Periods of believing one has died, or that the room is alive. Most of this resolves as the medicine clears. The participant comes back, integrates the material, and the experience lands as meaningful rather than pathological.
A psychotic break that has been triggered by ayahuasca looks different in three specific ways. The state does not end when the pharmacology does. The participant cannot bracket the experience even with strong support from facilitators or family. Reality testing remains impaired hours and then days after the ceremony. If a participant in the morning still believes they were in contact with discarnate entities and is acting on that belief in ways that endanger themselves or others, the situation is no longer integration. It is a psychiatric emergency, and the appropriate response is medical, not ceremonial.
Retreats that work this carefully will have, before the ceremony begins, an established relationship with a local clinic or hospital and a clear escalation pathway. Family members of someone in this situation should not wait for the retreat to handle it alone. Call the local emergency number, name the medicine, name the duration of symptoms, and request psychiatric evaluation. The framing matters because some emergency departments are unfamiliar with serotonergic crisis presentations and benefit from being told exactly what was ingested.
How Ethical Retreats Screen, and What to Look For
A discovery call that takes thirty seconds is a red flag. A discovery call that takes forty minutes and asks uncomfortable questions is the basic standard.
The screening protocols recommended in the ayahuasca clinical safety literature share a structure. A medical history covering cardiovascular conditions, seizure disorders, current medications, and any history of psychotic, manic, or major dissociative episodes. A psychiatric history covering personal and first-degree-relative diagnoses. A current-medication review with washout windows established in coordination with the participant’s prescriber for any serotonergic agent. A behavioral-health pass covering active suicidality, eating disorders, and substance dependence (Rossi et al., 2023; ICEERS, 2019).
The questions a careful retreat will ask:
- Have you ever been hospitalized for mental health reasons?
- Have you ever been told you have a psychotic, schizophrenic, or schizoaffective disorder, or bipolar I with manic features?
- Has any first-degree relative been diagnosed with the conditions above, hospitalized for mental illness, or treated with antipsychotic medication?
- Are you currently taking an SSRI, SNRI, TCA, MAOI, or lithium? Trazodone? St. John’s wort? Tramadol? Dextromethorphan?
- What is your blood pressure history? Have you had a cardiac event in the last year?
- Are you currently in active treatment for an eating disorder or addiction?
- Are you currently experiencing thoughts of suicide?
- Are you pregnant or trying to become pregnant?
The red flags in the other direction matter as much. A retreat that does not ask any of the questions above, that promises ayahuasca will “cure” any psychiatric diagnosis, that imports brew kits without medical infrastructure on site, that has no relationship with a local hospital, that pressures a hesitant participant toward a second ceremony, that frames psychiatric medication as a “block” the medicine will dissolve. Each one of those is grounds to walk away. The U.S. Embassy in Lima issued a 2025 health alert noting deaths and severe illness among Americans following ayahuasca consumption in unregulated Peruvian retreat settings (U.S. Embassy Lima, 2025). The alert is not an argument against ayahuasca. It is an argument against the lowest tier of provider, where most of the documented harm concentrates.

Feel deeply.
Show up fully.

About the Author
Yasha Shah is the founder of MahaDevi Ayahuasca, a retreat center in Colombia. He has been working with ayahuasca since 2017, with experience across hundreds of ceremonies as both a participant and retreat organizer. Trained within the Shipibo and Camsá traditions, his work bridges indigenous wisdom, harm-reduction principles, and practical integration for modern seekers. Yasha writes about ayahuasca, plant medicine, and psychedelics, covering integration, preparation, and harm reduction to help readers make informed and responsible decisions.
Frequently Asked Questions
Can ayahuasca trigger schizophrenia or psychosis?
Yes, in vulnerable people. The systematic review of published human cases concluded that ayahuasca-associated psychosis is rare in absolute terms but concentrates almost entirely in people with personal or family histories of psychotic or manic illness (dos Santos et al., 2017). The pharmacology activates the same receptor systems that misfire in psychosis, and in a brain already loaded for that pattern, the experience can become a triggering event rather than a contained ceremony. Screening exists to catch this.
Is ayahuasca safe if I have a family history of schizophrenia?
No. A first-degree relative with schizophrenia, schizoaffective disorder, or bipolar I with psychotic features is a standard exclusion criterion in clinical ayahuasca protocols and harm-reduction guidelines (Rossi et al., 2023; ICEERS, 2019). The heritability of schizophrenia is high enough, and the cost of triggering a first psychotic episode serious enough, that responsible retreats decline these participants. This is true even if you yourself have never had a psychiatric episode.
Can ayahuasca cure schizophrenia?
No. There are no clinical trials of ayahuasca as a treatment for schizophrenia, and there is no credible scientific path toward it. The mechanism that gives ayahuasca its therapeutic profile in other conditions is the same mechanism that destabilizes a schizophrenic brain. Anyone selling ayahuasca as a cure for schizophrenia is either uninformed or dishonest. Schizophrenia is treated by integrated psychiatric care, not by psychedelics.
Who should never take ayahuasca?
People with schizophrenia, schizoaffective disorder, or other primary psychotic illness. People with bipolar I with manic or psychotic features. People with a first-degree relative diagnosed with the above. People currently taking SSRIs, SNRIs, TCAs, MAOIs, lithium, trazodone, tramadol, or St. John’s wort, unless a careful washout has been coordinated with their prescriber. People with severe or uncontrolled cardiovascular disease. People who are pregnant. Each of these is a hard line, not a discussion point.
Can psychedelics help schizophrenia symptoms at all?
There is no current research supporting psychedelics, including ayahuasca, as a treatment for the positive or negative symptoms of schizophrenia. The 5-HT2A agonist class is broadly considered contraindicated in this population. People living with schizophrenia who experience comorbid depression, anxiety, or addiction sometimes hope that psychedelic-assisted therapies being studied for those conditions will become available to them. They almost certainly will not, for the same pharmacological reasons covered above.
How do reputable ayahuasca retreats screen for psychiatric conditions?
A serious retreat takes a full medical and psychiatric history during a discovery call before booking, asks specifically about personal and first-degree-relative psychiatric diagnoses, requests a current medication list, coordinates any serotonergic washout with the participant’s prescriber, and reserves the right to decline a participant whose risk profile is not appropriate (Rossi et al., 2023). If the screening process can be completed in less than a few thoughtful conversations, it is not screening. It is intake.
What is the difference between a spiritual experience and a psychotic break after ayahuasca?
A meaningful ceremony state ends when the pharmacology ends. The participant returns to baseline reality testing within hours, can describe the experience without acting on it as literal external fact, and integrates the material over days. A psychotic break does not end. The participant cannot bracket the content. Reality testing remains impaired the next morning and beyond. If the second pattern is present, the situation is a medical emergency and requires psychiatric evaluation, not more ceremony.
Can ayahuasca make anxiety or mental health worse instead of better?
Yes, especially in unsupervised settings or in people whose underlying condition was not appropriately screened. The largest survey of ayahuasca users to date, with more than 10,000 respondents, found that adverse mental health effects in the weeks or months following use were reported by 55.9% of participants, though most viewed those effects as part of a difficult growth process (Bouso et al., 2022). Non-supervised context and pre-existing psychiatric diagnoses were the strongest predictors of negative outcomes.
Conclusion
The honesty in this conversation is the protection. Ayahuasca is not a treatment for schizophrenia, and the people most likely to be harmed by it are the ones for whom the wellness internet has the fewest warnings. A careful retreat, a careful prescriber, and a careful family member are all asking versions of the same question: who has more to lose than to gain from this medicine.
For the seeker who reads this and recognizes their own history, the answer is not always sad. Sometimes it is a redirection toward a therapy that has actual clinical evidence behind it for their condition. Sometimes it is a hard “not now” rather than a permanent “no.” Sometimes it is a relief, because the question had been weighing on a person who had not had it asked of them with this much care before.
The medicine is real. The pharmacology is real. Screening exists for a reason.
That reason is the people it protects.


