Table of Contents
- 1 Ayahuasca for PTSD: What the Science, Veterans, and Risks Reveal
- 1.1 What Is Ayahuasca and How Does It Work?
- 1.2 Can Ayahuasca Treat PTSD? What the Research Says
- 1.3 How Ayahuasca Affects the Trauma Response in the Brain
- 1.4 Ayahuasca for Veterans: Combat PTSD and the Heroic Hearts Movement
- 1.5 What to Expect in an Ayahuasca PTSD Ceremony
- 1.6 Safety, Side Effects, and Who Should Not Take Ayahuasca
- 1.7 Ayahuasca vs MDMA, Psilocybin, and Ibogaine for PTSD
- 1.8 Choosing a Reputable Retreat and the Role of Integration
- 1.9 Frequently Asked Questions
- 1.10 Conclusion
- 1.11 References
Ayahuasca for PTSD: What the Science, Veterans, and Risks Reveal
| Topic | Quick Answer |
|---|---|
| Strongest PTSD evidence | 71.4% of evaluable combat veterans (5 of 7 per published correction) showed clinically significant PCL-5 reductions, sustained at follow-up (Weiss et al., 2023) |
| Proposed mechanism | 5-HT2A agonism + sigma-1 receptor + MAOI synergy; default mode network shift; BDNF elevation |
| Standard course | 3 to 6 ceremonies over a structured 1 to 2 week retreat with formal integration |
| Critical contraindications | SSRIs, SNRIs, MAOIs, lithium; uncontrolled hypertension; bipolar I; psychotic-spectrum disorders; pregnancy |
| Adverse-event rate | 2.3% of 10,836 global users required medical attention; serious events rare in screened populations (Bouso et al., 2022) |
| US legal status | DMT is Schedule I federally; Colorado decriminalized DMT under Prop 122 with healing centers in phased rollout; religious exemption for UDV / Santo Daime (Gonzales v. O Centro, 2006) |
PTSD is a brain change. Conventional first-line care, SSRIs and trauma-focused psychotherapy, helps many people and fails to fully resolve symptoms in many others. The literature on treatment-resistant PTSD has driven serious clinical interest in psychedelic-assisted approaches, with MDMA, psilocybin, and ayahuasca all under active investigation (Bahji et al., 2023). Below is what the science actually shows, what the risks actually are, and what someone considering ayahuasca for trauma should understand.
What Is Ayahuasca and How Does It Work?
Two plants. One brew. A pharmacology that should not work, and does.
Ayahuasca is a brewed Amazonian decoction made from two plants: the woody vine Banisteriopsis caapi and the leaf of Psychotria viridis (or, in some lineages, Diplopterys cabrerana). The viridis leaf contains N,N-dimethyltryptamine, or DMT, a powerful serotonergic psychedelic that the gut and liver normally break down within minutes of ingestion. The caapi vine contains β-carboline alkaloids, primarily harmine, harmaline, and tetrahydroharmine, that inhibit monoamine oxidase A long enough to let DMT cross into the bloodstream and the brain (Egger et al., 2024).
The result is an orally active psychedelic that takes effect in roughly 20 to 60 minutes and lasts four to six hours. The experience varies widely across people, doses, and settings. It can include intense visual imagery, somatic discharge, emotional release, contact with autobiographical memory, and, often, vomiting. The vomit is named in the Amazon and called la purga. It is not treated as a side effect. It is treated as part of the medicine.
That is the working definition for this guide. The deeper picture of the brew, the lineages, the chemistry, and the cultural context lives at the MahaDevi ayahuasca page. From here, the article focuses on what happens when this medicine meets PTSD.
Can Ayahuasca Treat PTSD? What the Research Says
The data is small. The signal is loud.
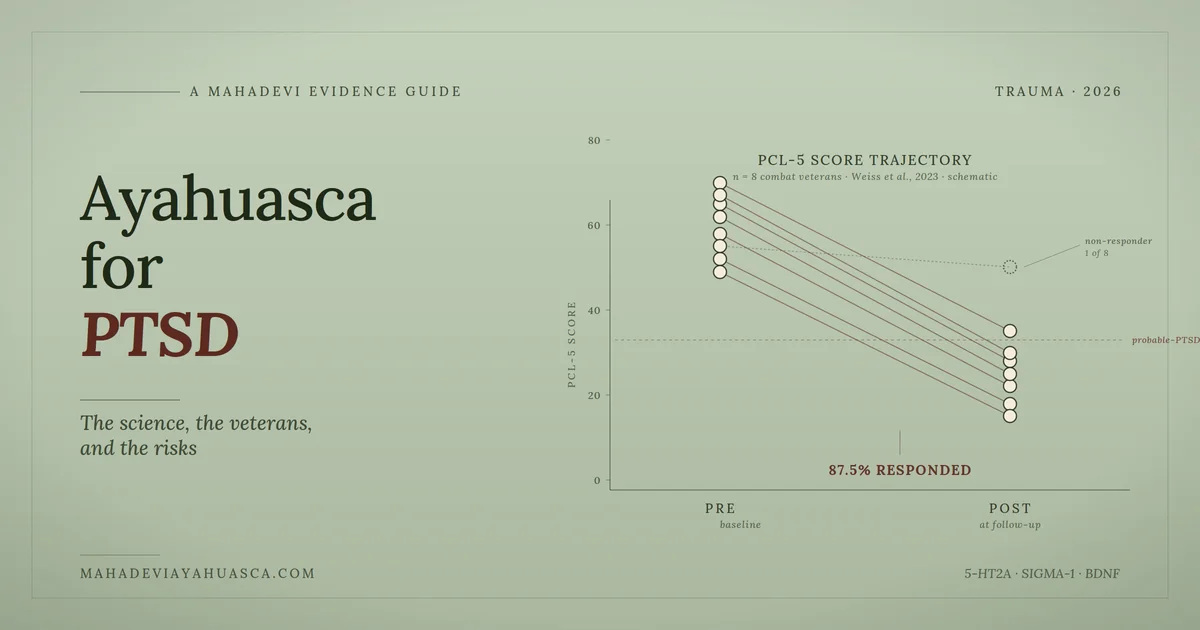
The strongest dedicated PTSD evidence comes from a 2023 mixed-methods case series of U.S. military combat veterans who attended a three-day ayahuasca intervention. Per the published correction, 71.4 percent of evaluable participants (5 of 7) demonstrated reliable or clinically significant reductions in PCL-5 (PTSD Checklist for DSM-5) symptom severity, sustained at follow-up (Weiss et al., 2023). The sample is tiny. The effect size is large. The study is best read as a hypothesis-generating signal rather than confirmation of efficacy, and it is consistent with what observational data has been suggesting for years.
A 2023 systematic review of the broader ayahuasca literature found consistent evidence of beneficial effects on depression, anxiety, substance use disorders, and PTSD across clinical trials, observational studies, and surveys, with a generally favorable safety profile in screened populations (Duarte et al., 2023). A 2024 meta-analysis of 126 articles on psychedelic therapy for mental disorders placed ayahuasca’s effect on depression and anxiety at Hedges’ g = −1.34, second only to psilocybin among the psychedelic agents studied (Yao et al., 2024). PTSD-specific effect sizes were not separately calculable in that analysis because the trial pool is still too thin.
The Global Ayahuasca Survey, the largest dataset on the brew, captured 11,912 international consumers with prior diagnoses. Among those with depression, 78 percent reported symptoms “very much improved” or “completely resolved” after ayahuasca use; 70 percent of those with anxiety reported similar improvement (Sarris et al., 2021). Self-report data has known limits and does not replace controlled trials. It does describe the territory the controlled trials are now mapping.
Active clinical research continues at Johns Hopkins (Johns Hopkins, 2024), Imperial College London (Imperial College London, 2025), and through ICEERS and MAPS (ICEERS, 2023)(MAPS, n.d.). The honest summary: the ayahuasca PTSD literature sits roughly where the MDMA PTSD literature was fifteen years ago. Small studies. Large signals. Growing institutional interest. Not yet the regulatory infrastructure to call it a treatment.
How Ayahuasca Affects the Trauma Response in the Brain
The brain is not erasing the memory. It is changing how it holds it.
The most coherent mechanistic account of ayahuasca’s effect on traumatic memory was proposed by Inserra in 2018. The hypothesis runs as follows. DMT is a potent agonist at the sigma-1 receptor, a chaperone protein that regulates neuroplastic processes at the interface between the endoplasmic reticulum and the mitochondria. Sigma-1 activation, combined with β-carboline MAO inhibition, may facilitate the retrieval of repressed traumatic memories, destabilize them through neuroplasticity-promoting pathways including BDNF and neurogenesis, and allow them to be reconsolidated into a less reactive form (Inserra, 2018).
Several converging findings support the pathway. A double-blind RCT showed that a single ayahuasca dose significantly elevated serum BDNF in both depressed patients and healthy controls, with elevation associated with antidepressant response (de Almeida et al., 2019). Functional imaging shows that 24 hours post-ceremony, the salience network strengthens its anterior cingulate connectivity while the default mode network reduces posterior cingulate connectivity, a pattern that maps onto reduced rumination and improved emotional integration (Pasquini et al., 2020). A placebo-controlled trial also found significant C-reactive protein reduction at 48 hours, suggesting an immunomodulatory dimension to the antidepressant effect (Galvão-Coelho et al., 2020).
Pulled together: ayahuasca produces a brief, intense window of neuroplasticity. Memories frozen in the threat-response circuitry become accessible. Under that altered state, with appropriate facilitation, the memory can be re-encoded with new emotional and somatic information. The traumatic event is not forgotten. It loses its capacity to ambush.
Ayahuasca for Veterans: Combat PTSD and the Heroic Hearts Movement
What works for one trauma profile does not always carry across to another. Veterans are a specific case.
The veteran population has driven a disproportionate share of the public conversation around psychedelic therapy for PTSD. Combat trauma is often diagnostically clean, the failure rate of conventional VA care is high, and the cohort includes people willing to travel to a jungle in Peru or a clinic in Mexico when the alternative is another decade of partial response. Organizations like the Heroic Hearts Project and VETS Inc. have channeled hundreds of veterans into ayahuasca and ibogaine retreats, and journalism on the trend has reached mainstream outlets including the New York Times (Londoño, New York Times, 2020). The 2018 documentary From Shock to Awe brought the same story to a wider audience.
The Weiss case series is the most rigorous data point inside the veteran cohort specifically. The published correction reports 5 of 7 evaluable participants (71.4 percent) showed clinically meaningful PCL-5 reductions sustained at follow-up. The qualitative themes pointed toward emotional release, self-forgiveness, and reconnection with parts of the self that combat had walled off (Weiss et al., 2023).
For veterans whose PTSD also involves traumatic brain injury, parallel work on ibogaine has shown rapid improvements in disability, PTSD, depression, and anxiety in U.S. Special Operations personnel treated with magnesium-buffered ibogaine in Mexico (Cherian et al., 2024). Ibogaine is not ayahuasca and the cardiac risk profile is materially different, but the convergence is worth noting. Two distinct psychedelic agents, two clinically observed signals, in the same hard-to-treat population.
The veteran data also surfaces a critical caveat. Combat PTSD is often single-event repeated. Childhood abuse, sexual trauma, and complex PTSD have different memory architectures and the dedicated trial evidence has not caught up. Observational and survey data is broadly favorable; controlled trials in those populations remain to be done.
What to Expect in an Ayahuasca PTSD Ceremony
A ceremony is not a clinical procedure and it is not a vacation. The form varies by lineage, but the essential arc is recognizable across most traditions and most well-run modern retreats. A typical ceremony unfolds roughly as follows:
- Days before: la dieta. Dietary, behavioral, and often sexual restriction. Most traditions exclude red meat, pork, alcohol, recreational drugs, fermented foods, salt, sugar, and tyramine-rich foods that interact with the MAOI in the brew. Many lineages add intention-setting work and conversations with the facilitator.
- Hour 0: opening the space. Participants gather in a maloca or ceremonial space after dark. Facilitators open with prayer, song, or silence depending on lineage. Cups of medicine are served individually.
- Hours 0 to 1: onset (mareación). First effects begin within 20 to 60 minutes. Visual textures shift. The body begins to feel the medicine. Many participants experience an initial wave of nausea or anxiety.
- Hours 1 to 4: the peak. The strongest part of the experience. Visual imagery, emotional release, autobiographical memory, somatic shaking, and stretches of stillness. This is when most therapeutic processing occurs.
- Throughout: la purga and the icaros. Vomiting and diarrhea are common and traditionally framed as the purge. Songs called icaros, sung by the facilitators, function as therapeutic instruments and are described in research as precision tools used to scan and adjust each participant’s process (Gonzalez et al., 2021).
- Hours 4 to 6: descent and close. Effects taper. Facilitators close the ceremony. Most participants rest until dawn.
- The morning after: sharing circle. Most retreats hold a structured sharing the next morning. Skilled facilitators do not interpret. They listen.
The variance across people and ceremonies is wide. A retreat designed for trauma work plans for that.
Safety, Side Effects, and Who Should Not Take Ayahuasca
The medicine has a toxicology. The honesty is part of the safety.
The largest dataset on adverse effects comes from the Global Ayahuasca Survey of 10,836 users across more than fifty countries. Acute physical adverse effects, primarily vomiting, occurred in 69.9 percent. Only 2.3 percent required medical attention. Adverse mental health effects in the weeks or months following use were reported by 55.9 percent, with around 88 percent resolving naturally or treated by the user as part of growth (Bouso et al., 2022). The risks that exist in screened populations are concrete and worth naming.
Medications that contraindicate ayahuasca:
- SSRIs (sertraline, paroxetine, fluoxetine, citalopram, escitalopram and others)
- SNRIs (venlafaxine, duloxetine)
- Tricyclic antidepressants and trazodone
- MAOIs (phenelzine, tranylcypromine)
- Lithium
- Tramadol, dextromethorphan, meperidine
- St. John’s wort and 5-HTP supplements
- MDMA, cocaine, amphetamines
- Sympathomimetic decongestants (pseudoephedrine, ephedrine)
Combining ayahuasca with serotonergic medications carries a serious risk of life-threatening serotonin syndrome (Callaway & Grob, 1998)(Malcolm & Lee, 2018). Reputable retreats require a documented washout: typically four to six weeks for most SSRIs and six weeks or longer for fluoxetine. Stopping psychiatric medication is a conversation with the prescriber, never a unilateral decision. For the full breakdown of agents and washout windows, see our SSRI and MAOI interaction guide.
Foods to avoid in the days before ceremony (tyramine reaction risk with MAOIs): aged cheese, cured and aged meats, fermented soy products (soy sauce, miso, tempeh), fermented vegetables, draft and unpasteurized beers, broad beans (fava beans), and overripe or fermented fruit.
Medical and psychiatric conditions that contraindicate ayahuasca:
- Uncontrolled hypertension, recent cardiac events, significant arrhythmia history (in controlled study, only the diastolic rise of about 9 mmHg at 75 minutes was statistically significant; the parallel systolic and heart-rate rises were moderate and non-significant) (Riba et al., 2003). See ayahuasca and blood pressure and ayahuasca and the heart for the deeper guides.
- Personal or family history of psychotic-spectrum disorders (schizophrenia, schizoaffective disorder)
- Bipolar I disorder, particularly with documented manic episodes
- Active suicidality without therapeutic infrastructure in place
- Pregnancy (animal models show abortifacient and teratogenic effects at higher doses) (White et al., 2024)
- Severe liver or kidney disease
- Epilepsy with poorly controlled seizures
Psychotic episodes following ayahuasca are rare in the broader population, with one systematic review estimating prevalence in religious-use populations at 0.0032 to 0.096 percent of servings, but personal or family history of psychosis or mania substantially increases the risk (dos Santos et al., 2017). ICEERS and clinical safety guidelines treat psychotic-spectrum and bipolar I diagnoses as exclusions in non-clinical retreat settings (ICEERS, 2024)(Rossi et al., 2023).
Ayahuasca vs MDMA, Psilocybin, and Ibogaine for PTSD
The four agents most often discussed for PTSD-related work are ayahuasca, MDMA, psilocybin, and ibogaine. Each carries a different mechanism, evidence base, setting, and risk surface. The comparison below is intentionally simplified for orientation. None of these substitute for medical advice from a qualified prescriber.
| Feature | Ayahuasca | MDMA | Psilocybin | Ibogaine |
|---|---|---|---|---|
| Legal status (US) | DMT Schedule I; UDV / Santo Daime religious exemption; decriminalized in Colorado (Gonzales v. O Centro, 2006)(Colorado Prop 122, 2022) | Schedule I; FDA review pending; expanded access in some jurisdictions | Schedule I federally; legal regulated programs in Oregon and Colorado (Oregon Measure 109, 2020) | Schedule I; legal in Mexico, New Zealand, parts of Canada |
| Evidence quality (PTSD) | One mixed-methods veteran case series (n=8); broad observational data (Weiss, 2023) | Largest base; completed Phase 3 trials; strongest PTSD-specific signal (Bahji et al., 2023) | Strong depression evidence; PTSD evidence emerging | Veteran case series with TBI / PTSD; cardiac safety remains the principal concern (Cherian et al., 2024) |
| Session duration | 4 to 6 hours per ceremony; typically 3 to 6 ceremonies | 6 to 8 hours; typically 3 dosing sessions | 4 to 6 hours; typically 1 to 3 sessions | 24 to 36 hours including post-acute care; typically 1 session |
| Primary indication | Depression, anxiety, PTSD, substance use disorder | PTSD (lead indication) | Depression (lead indication); existential distress; addiction | Opioid use disorder; emerging TBI / PTSD work in veterans |
| Key risks | SSRI / serotonergic interactions; cardiovascular load; psychosis risk in vulnerable | Hyperthermia; cardiovascular; serotonergic interactions; SSRI attenuation | Difficult experiences; SSRIs typically attenuate effect; psychosis risk in vulnerable | QTc prolongation, torsades de pointes; cardiac arrest; mandatory cardiac screening |
The comparison is not a ranking. The right answer for a given person depends on diagnosis, history, medications, geography, and what the person is actually seeking from treatment. A 2023 meta-analysis of psychedelic-assisted therapies across these agents concluded that all four show significant therapeutic effects, with psilocybin showing the largest depression effect size and MDMA the strongest specific PTSD signal, while ayahuasca demonstrates broad efficacy across mood, anxiety, and trauma domains (Bahji et al., 2023).
Choosing a Reputable Retreat and the Role of Integration
The quality of the retreat determines the quality of the work. The market is unregulated and the variance is enormous. A short vetting checklist filters most of the noise. For PTSD work specifically, every item on this list matters.
10-point retreat vetting checklist:
- Medical screening before deposit. Detailed intake covering medications, psychiatric history, cardiovascular profile, and family history. Centers willing to decline applicants are taking screening seriously.
- Required medication washout protocols. Documented washout periods coordinated with the participant’s prescriber.
- On-site or on-call medical staff. Physician available, basic emergency medications accessible, clear protocols for psychiatric and cardiac events.
- Lineage and training transparency. The retreat names where its tradition comes from, who its facilitators trained with, and how the brew is prepared.
- Trauma-informed facilitation. Facilitators with direct experience holding space for trauma survivors, ideally with formal training in psychedelic-assisted therapy or somatic trauma work.
- Small group size. High facilitator-to-participant ratio. Ten participants per facilitator is too many for trauma work; three to four is appropriate.
- Pre-retreat preparation. Structured dieta guidance, intention setting, and pre-retreat calls with the facilitation team.
- On-retreat integration. Daily integration sessions, sharing circles, and one-on-one time with facilitators built into the schedule.
- Post-retreat integration support. A defined integration arc through the retreat’s coaches or a referral network of psychedelic-informed therapists.
- Reciprocity and ethics. Documented contributions to indigenous communities of origin and clear ethical guidelines around touch, consent, and facilitator-participant boundaries. ICEERS publishes a good-practice guide participants can use as a baseline reference (ICEERS, 2019).
Integration is where the healing lives. The peer-reviewed literature treats integration as a standalone clinical practice, not an optional add-on, and the largest qualitative study of post-ayahuasca integration found it is experienced as challenging, long-term, and communal rather than primarily individual (Gorman et al., 2021)(Cowley-Court et al., 2023). For PTSD specifically, this is where the brief neuroplastic window opened by ceremony either gets used or gets wasted. For the trauma-informed approach to integration, see our trauma-informed care framework.

Feel deeply.
Show up fully.

About the Author
Yasha Shah is the founder of MahaDevi Ayahuasca, a retreat center in Colombia. He has been working with ayahuasca since 2017, with experience across hundreds of ceremonies as both a participant and retreat organizer. Trained within the Shipibo and Camsá traditions, his work bridges indigenous wisdom, harm-reduction principles, and practical integration for modern seekers. Yasha writes about ayahuasca, plant medicine, and psychedelics, covering integration, preparation, and harm reduction to help readers make informed and responsible decisions.
Frequently Asked Questions
Is ayahuasca legal for PTSD treatment in the United States?
No, not as a treatment. DMT, the active psychedelic in ayahuasca, is Schedule I under federal law (DEA, 2024). The brew has no FDA-approved indication for PTSD. A 2006 Supreme Court ruling allows religious use by the UDV and Santo Daime churches under RFRA (Gonzales v. O Centro, 2006). Colorado decriminalized DMT for adults 21+ under Proposition 122, with licensed healing centers in phased rollout (Colorado Prop 122, 2022). Most therapeutic ayahuasca work for trauma takes place at retreats in Peru, Brazil, Colombia, or Costa Rica.
Can you take ayahuasca if you are on antidepressants (SSRIs or MAOIs)?
No. Combining ayahuasca with SSRIs, SNRIs, tricyclics, or pharmaceutical MAOIs carries a serious risk of life-threatening serotonin syndrome (Callaway & Grob, 1998). Reputable retreats require documented washout, typically four to six weeks for most SSRIs and six weeks or longer for fluoxetine due to its long half-life. Stopping antidepressant medication is a decision made with the prescribing clinician, never unilaterally and never to attend a retreat. A retreat that does not require medication disclosure is a retreat that does not understand its own risk surface.
Can you take ayahuasca with high blood pressure or BP medication?
Uncontrolled hypertension is a contraindication. The most rigorous controlled study found a statistically significant diastolic rise of about 9 mmHg above placebo at 75 minutes; the parallel systolic and heart-rate rises were moderate and non-significant in the same trial (Riba et al., 2003). People on antihypertensive medication should disclose all prescriptions to the retreat and to their prescriber before considering ceremony. Some BP medications interact with the MAOI alkaloids in ayahuasca. A cardiac history including arrhythmia or recent cardiac events is a firm exclusion under most reputable safety guidelines (ICEERS, 2019). See also ayahuasca and blood pressure.
How long do the effects of ayahuasca last?
Acute effects begin within 20 to 60 minutes of ingestion and last four to six hours, with the peak typically falling between hours one and four. Subacute neurobiological effects extend longer. Functional imaging shows brain network changes still detectable 24 hours after ceremony (Pasquini et al., 2020), and inflammatory marker reductions persist at 48 hours (Galvão-Coelho et al., 2020). The therapeutic window for integration work, when the brain is most receptive to new patterns, is generally considered to extend two to four weeks following ceremony.
Is ayahuasca addictive or can it cause psychosis?
Ayahuasca is not pharmacologically addictive and the experience is intense enough that compulsive use is rare. Several observational studies have actually found ayahuasca use associated with reductions in alcohol and other substance use among long-term ceremonial drinkers (Duarte et al., 2023). Psychotic episodes are also rare in the broader population, with one systematic review estimating prevalence in religious-use populations at 0.0032 to 0.096 percent of servings (dos Santos et al., 2017). The risk concentrates sharply in people with personal or family history of psychotic-spectrum disorders or bipolar I, which is what screening exists for.
Has anyone died from ayahuasca?
Deaths attributed to ayahuasca are rare but real. Documented cases tend to involve drug interactions, undisclosed medical conditions, unscreened cardiac vulnerability, or adulterated brews containing additional substances. The Global Ayahuasca Survey of 10,836 users found 2.3 percent required medical attention; serious adverse events were uncommon in screened populations (Bouso et al., 2022). A systematic toxicity review found ayahuasca generally safe in healthy populations in controlled settings, with serious adverse effects rare (White et al., 2024). Risk concentrates in unscreened settings and in people with the contraindications named above.
What is the difference between ayahuasca and ibogaine for PTSD?
Different molecules, different mechanisms, different risk profiles. Ayahuasca acts primarily via 5-HT2A serotonin receptor agonism, sigma-1 activation, and MAO inhibition; the experience runs four to six hours per ceremony, typically across multiple ceremonies. Ibogaine acts at multiple receptor systems and produces a 24 to 36 hour experience, usually a single dose, with magnesium-buffered protocols showing rapid PTSD and depression improvement in veteran populations with TBI (Cherian et al., 2024). Ibogaine carries a meaningfully higher cardiac risk profile than ayahuasca and requires mandatory cardiac screening including QTc measurement.
How do I find a reputable ayahuasca retreat for PTSD?
Use the ten criteria above as a starting filter. The non-negotiables for trauma work are medical screening before payment, required medication washout protocols, on-call medical staff, trauma-informed facilitation, small group size, structured pre-retreat preparation, daily on-retreat integration, and a defined post-retreat integration plan. Add lineage transparency and documented reciprocity with indigenous communities. ICEERS publishes a good-practice guide that participants can use as an independent reference point against any retreat’s claims (ICEERS, 2019). The conversation that matters is with the retreat itself, before any commitment.
Conclusion
The literature on ayahuasca and PTSD is younger than it needs to be. The signal is consistent enough across small trials, large observational datasets, and centuries of indigenous practice that ignoring it is no longer the reasonable position. Acting on it without screening, integration, and a sober understanding of the risks is also not the reasonable position.
For someone living with PTSD, the relevant questions are concrete. Are your medications compatible with washout. Is your cardiovascular profile clear. Is there a history of psychotic-spectrum illness in your family. Do you have therapeutic support to integrate what comes up. Have you found a retreat with the screening, lineage transparency, and trauma-informed facilitation that the work demands.
The medicine is not magic. It is pharmacology meeting context meeting the brain’s own capacity to heal when the right window opens. The window is what ceremony provides. The healing is what the participant does with it.
References
ICEERS. (2023). Ayahuasca | International Center for Ethnobotanical Education, Research & Service.
Imperial College London Centre for Psychedelic Research. (2025). Imperial College London.


